
Projects funded from Dry July 2017
Thanks to funds raised from Dry July 2017, Shoalhaven Cancer Care Centre have been able to fund:
- NEW magazines throughout the patient spaces in the Centre
- Children’s Creativity Packs for children accompanying adults to appointments
- 2018: Living Well After Treatment Workshops
- Music delivered via iPad and speaker, while patients undergo Radiation Therapy treatment
- Colour me Calm Mindfulness Resource Kits for Chemotherapy patients
- Welcome to Cancer Services video for patient viewing (in development)

Projects funded from Dry July 2017
Thanks to funds raised from Dry July 2017, Wollongong Hospital (Illawarra Cancer Care Centre) have been able to fund the following projects:
- NEW magazines throughout the patient spaces in the Illawarra Cancer Care Centre and Cancer Inpatient Ward
- Children’s Creativity Packs for children accompanying adults to appointments
- 2018: Patient and Carer Tai Chi Program
- 2018: Living Well After Treatment Workshops
- Large Pots housing palms outside the Level 2 entrance to the Illawarra Cancer Care Centre
- Music, delivered via iPad and speaker, while patients undergo Radiation Therapy treatment
- Colour me Calm Mindfulness Resource Kits for Chemotherapy patients
- A Hydration Station in the Radiation Therapy patient waiting space (launching...
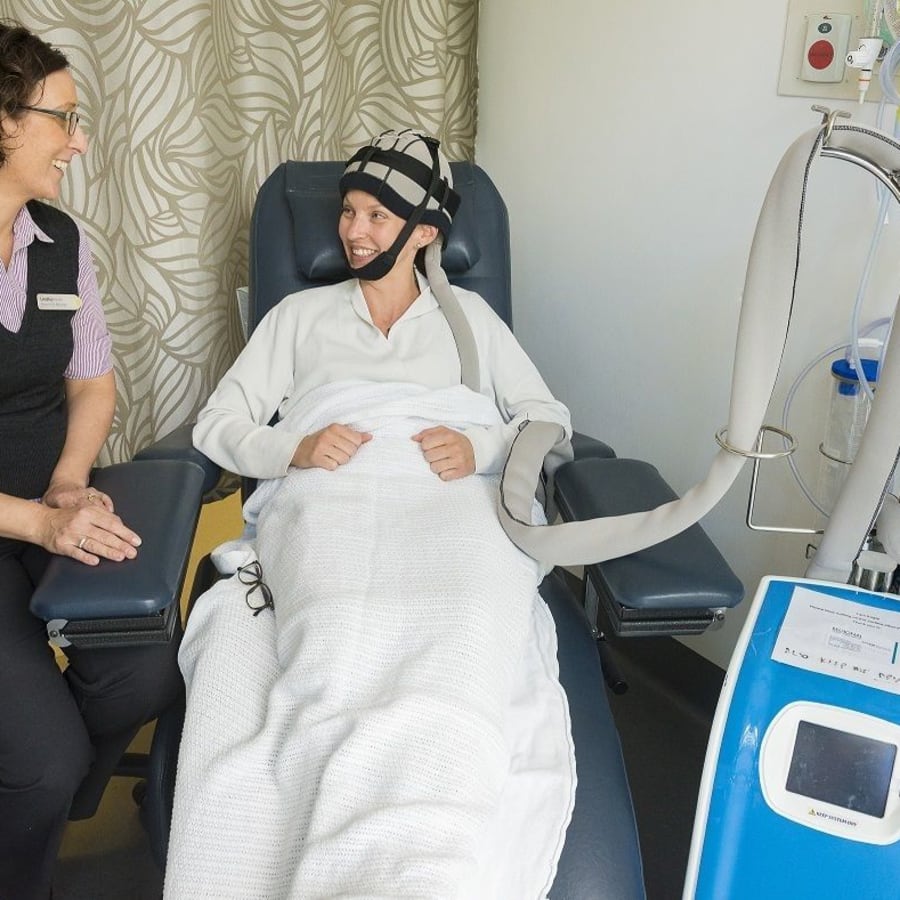
Paxman Scalp Cooling Unit for Chris O'Brien Lifehouse
Nurse Unit Manager Lindley Randle from Chris O'Brien Lifehouse's Day Therapy Unit was delighted to be able to purchase a Paxman Scalp Cooling Unit designed to reduce and prevent hair loss during selected chemotherapy treatments. This was made possible through Dry July funding.
For patients who meet the requirements to use the machine and who are distressed by the idea of losing their hair (and ‘looking like someone with cancer’), scalp cooling provides an opportunity to maintain the majority of their hair and to reduce the emotional and psychosocial burden of treatment.

Patient Transport Vehicle for Brisbane Patients
Every year the Leukaemia Foundation helps more than 750 families from regional and rural Australia by providing free accommodation and transport in capital cities so they can access life-saving treatment for blood cancer.
Our patient transport vehicles, driven by trained volunteers, help thousands get to and from medical appointments, covering more than one million kilometres each year. This means that patients whose immune systems are often too weak to take public transport or a taxi can rely on friendly, on-time drivers to deliver them to treatment and back home again, safe and sound.
For the Livara family of five from Blackwater in Central Queensland, having these services available means the family can worry less about practical...

PCFA Receives a Dry July Foundation Grant
The Dry July Foundation was pleased to award Prostate Cancer Foundation of Australia (PCFA) a grant in 2017 towards the Prostate Cancer Specialist Nursing (PCSN) program.
Prostate cancer is too frightening to face alone. Our expert nurses provide coordinated support throughout the entire prostate cancer journey; taking into account physical, emotional, psychological and social needs of men and their families.
Patients often tell PCFA that they need "an opportunity to talk through [their] diagnosis beyond what is available in a standard 15-minute consult with a urologist". Specialist nurses can help patients and their families to understand their diagnosis, what to expect and connect them with services to address the challenges that they...

Exercise Therapy at Barwon Health
Warrnambool resident Tony always considered himself fit and healthy, so he wasn’t concerned when he started experiencing unexplained tiredness and blood in his urine. His son, however, was not happy with this assumption and urged Tony to see his GP.
After a number for tests and specialist appointments, the 65-year-old was called into the clinic to meet with his doctor.
“As soon as I looked at her, I felt a shiver down my spine,” he said.
“She sat me down and said I had Acute Leukaemia. You could have knocked me down with a feather.
“She told me with about two months of chemo I had about a 40 per cent chance of remission.”
However, all Tony could think about was his family.
“I just didn’t know how to deal with this,” he said.
“I thought to...
Saving patients travel time and costs at The Royal Melbourne Hospital
On behalf of the staff and patients at The Royal Melbourne Hospital, thank you so much for the grant for the oncolology telemedicine room. The project is now complete.
The telehealth team were honoured to be offered the opportunity to facilitate innovation of care delivery for oncology outpatients through funding from the Dry July Foundation.
With the generous support of the Dry July donation we have been able to purchase several key pieces of infrastructure to enable easy access to videoconferencing for our oncology patients.
In addition to telehealth being available in every outpatient room, the oncology team can also perform multidisciplinary meetings in their usual group meeting rooms via videoconference. Professor Kate Drummond...

First patient to be given the gift of saving their hair
Thanks to funds raised by last year's Dry July participants, St Vincent's Hospital in Melbourne have purchased one of the first scalp cooling caps available to public patients in Victoria.
The cap reduces the risk of hair loss during chemotherapy by decreasing scalp temperature and blood flow to hair follicles.
Afaf Shenouda couldn’t believe her luck when she was told she would be the first patient to be treated with a scalp cooling cap during her chemotherapy treatment at St Vincent’s.
‘How lucky am I to receive this treatment?’ Afaf says. ‘I’m so grateful to the donors who have given me the opportunity to keep my hair.’
‘It feels and sounds like rain, like it’s hailing on my head,’ Afaf explains, when the cap was first turned on. Afaf...

Glenda's Story - Barwon Health Foundation Volunteer Gives Back
At 55, Glenda was a fit and healthy marketing consultant relishing in the joys of becoming a grandmother for the first time. It was the discovery of a small, painless lump in her throat that changed Glenda’s life.
“Eighteen days after surgery to remove the lump I had a massive bleed requiring hospitalisation to cauterise it. As I was going under, I was told I might not live through the operation but thankfully I did,” Glenda said.
“I had 35 rounds of radiation therapy simultaneously with chemotherapy over seven weeks. After the tonsil was removed, I had a PEG tube inserted into my stomach to allow me to have a high protein liquid food. It remained there for eight months. During this period I was unable to eat solid foods for most of...










